Athelas RCM for Federally Qualified Health Centers
The Only RCM Platform Designed for How FQHCs Truly Operate
Medicaid changes are accelerating. Is your revenue cycle ready?
New federal rules are making it harder for FQHCs to keep patients enrolled and harder for staff to keep up.
Athelas wants to help
We’re working directly with FQHCs to:
Reduce churn
Catch revenue at risk
Tailored, in-person support
Keep patients covered
Get the most out of AI-powered tools
Why FQHCs Are Choosing Athelas RCM
Wade Meier | Co-Founder, Meier & Marsh
Real-time Medicaid eligibility tracking
Automatically flags upcoming redeterminations, so no renewal falls through the cracks.
Patient outreach, fully automated
Send personalized texts, phone calls, or messages to guide patients through renewal without extra work for your staff.
Conversational AI that walks patients through the process
No portal logins. No paperwork confusion. Just seamless step-by-step guidance, right from their phones.
Revenue cycle automation built for FQHCs
From claim scrubbing to resubmission, our platform adjusts as rules change, so you don’t lose a dime to avoidable denials.
Hands-on partnership
Our team runs free financial health analyses, offers grant writing support, and helps you stay ahead of policy changes, no matter what’s next out of D.C.
Complimentary Financial Health Analysis
We’ll review two years of your billing data at no cost to identify:
Revenue at risk under new Medicaid rules
Gaps in eligibility tracking and follow-up
Opportunities for faster reimbursement
Grant and funding potential you may be missing
No strings. No pressure. Just a clear picture of where you stand and ways you can improve.
FQHC Case Study: Korean Community Services Boosts Annual Revenue by $4.5M with Athelas RCM
When new Medicaid rules started impacting enrollment at KCS, their team turned to Athelas to help keep care accessible amidst the policy shifts. They were able to:
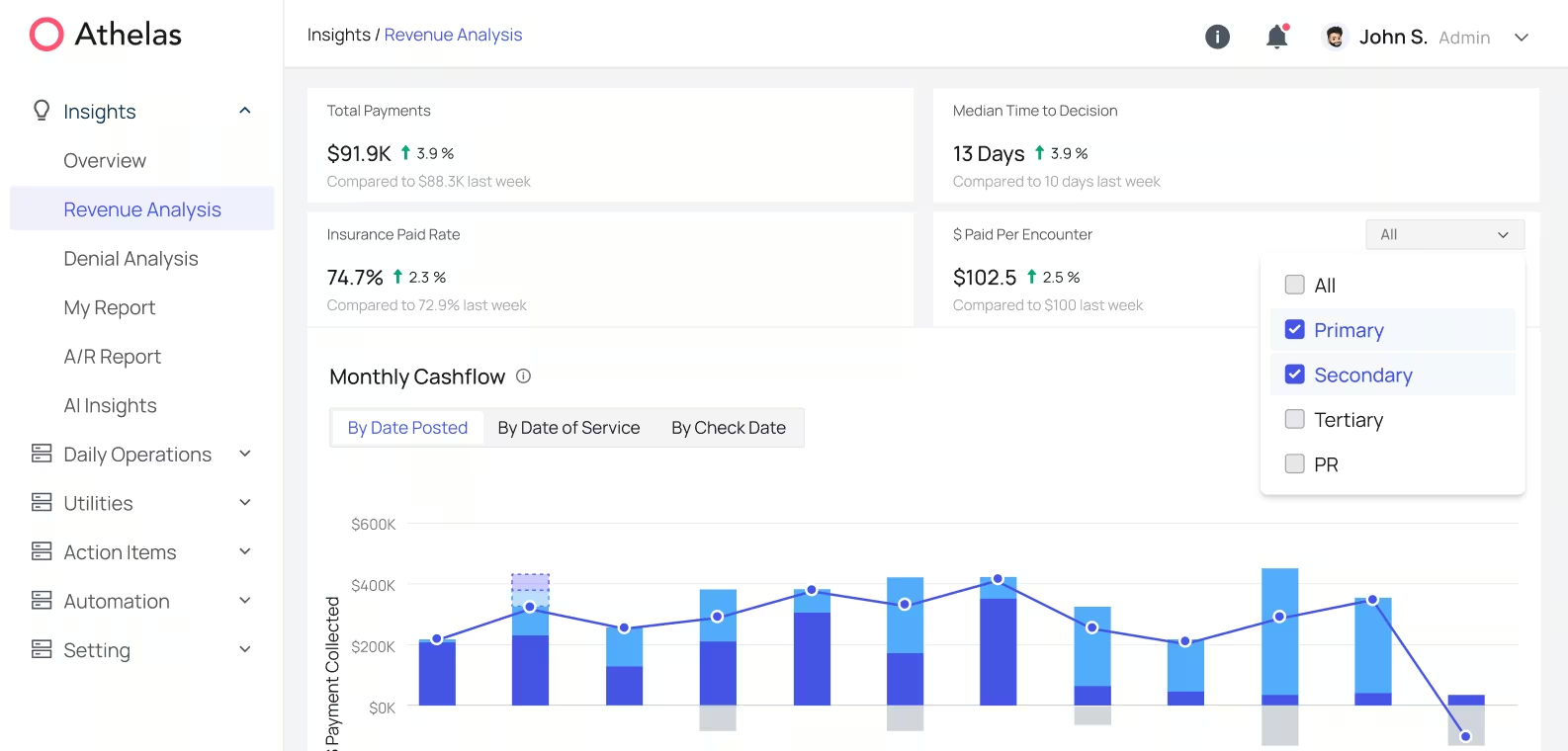
$372K
Gain $372K in monthly
revenue
96%
Obtain a 96% claims
reconciliation rate
$410K
Recover $410K from
unclosed encounters
4,500+
Resubmit 4,500+
denials in 60 days
12%
Increase average collected
per claim by 12%
1,200+
Save 1,200+ hours
monthly
Kay Ahn, MA | Chief Operating Office
With structured automation and a dedicated Athelas recovery team, KCS now resolves claims faster, captures more revenue, and maintains confidence through shifting Medicaid landscapes.
RCM Built for FQHCs. Backed by AI. Supported by Real People
Athelas is the only all-in-one platform powering over 400,000 providers across the country. For RCM FQHCs, we go further. We offer:






UDS reporting & sliding fee schedule support
Grant writing guidance & strategy
In-person site visits and staff training
AI tools that actually save your team time
Athelas offers FQHC-focused expertise and partnership.
Frequently Asked Questions
Athelas isn’t just a clearinghouse or outsourced billing shop; we combine AI automation, Medicaid eligibility intelligence, and a hands-on recovery team that works directly with your staff. We don’t wait for denials; we prevent them, track eligibility in real time, and intervene with patients long before revenue is at risk.
Our platform automatically identifies upcoming renewal deadlines, flags high-risk patients, and triggers multichannel outreach (text, phone, automated agent). Patients receive step-by-step assistance guided by conversational AI, meaning your front desk and outreach teams no longer have to chase down paperwork or portal logins.
Yes. Athelas integrates with all major FQHC EHRs (eClinicalWorks, NextGen, Epic Community Connect, Athena, etc.). Eligibility data, claim status, resubmissions, and reporting sync seamlessly without disrupting your current workflows.
On average, FQHC partners see:
- 10–20% more collected per claim
- Faster days in A/R
- Significant drops in avoidable denials
- Recovered revenue from old encounters, backlogs, and unresolved denialsCase study results, like KCS’s $4.5M annual revenue lift, represent what’s possible with full implementation and our recovery team engaged.
Our RCM workflows are built for FQHC reporting standards. Athelas supports:
- UDS encounter capture and compliance
- Sliding fee schedule logic
- PPS/APM billing models
- Managed care carve-outs
Your reporting team gets cleaner data and fewer manual fixes at month-end.
Every FQHC gets a dedicated RCM team, including onsite visits, ongoing training, reimbursement strategy sessions, and live account managers. We also provide free financial health analyses, grant support, and policy-change updates so you’re always ahead of federal and state shifts.
Yes. Our Recovery Team specializes in:
- Backlogged denials and unclosed encounters
- Aged A/R cleanup
- Underpaid claims
- Retroactive coverage gaps
We run full audits and handle resubmissions, often reclaiming revenue centers assumed lost.
Absolutely. Athelas is built to meet HIPAA, HITECH, Medicaid, and state-level eligibility requirements. All PHI stays encrypted end-to-end, and our AI models are audited for fairness and compliance, especially around vulnerable populations served by FQHCs.
Most FQHCs go live in 6 weeks. Athelas handles the heavy lifting: data mapping, integration setup, eligibility sync, and partners closely with your billing and front-desk teams to ensure a smooth transition with zero downtime.
- Access to your EHR/PMS for syncing encounters and eligibility
- Historical billing data for your complimentary financial analysis
- A point of contact from your operations or billing team
Athelas handles everything else, including staff training, outreach scripting, and claim workflow configuration.
Get Ahead of the Curve
Athelas FQHC specialists are on standby. We’ll walk you through what other centers are doing, and how we can serve as your dedicated partner in safeguarding Medicaid continuity, strengthening financial stability, and supporting community-centered care.

