The Mid-Market Playbook for Cleaner Claims & Faster Cash
A practical blueprint for specialty practices and multi-location groups to reduce denials, get paid faster, and lighten admin load with Athelas RCM.
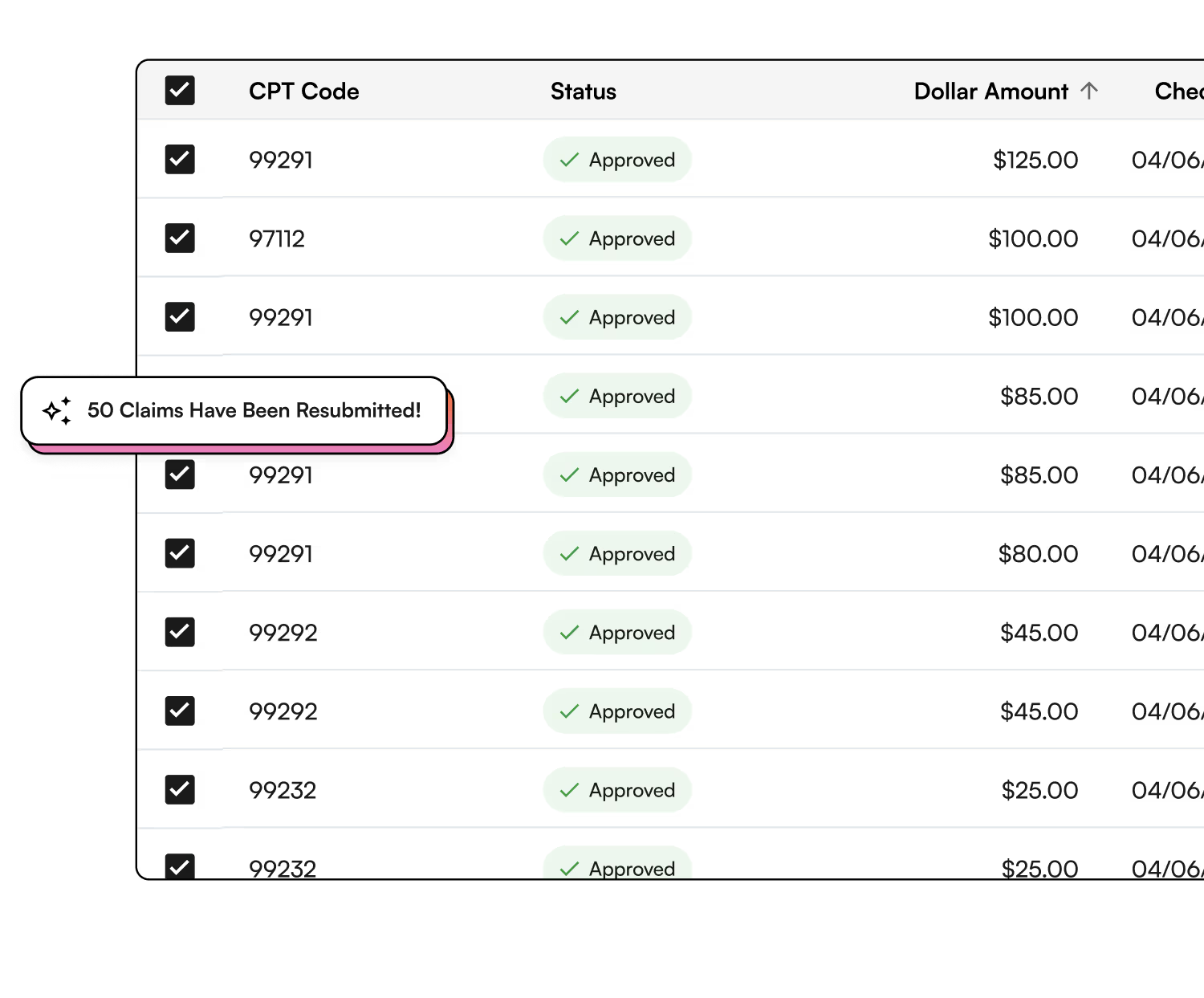
If your revenue cycle needs manual triage, it’s broken.
Mid-market practices don’t have enterprise headcount or an enterprise-level tolerance for delayed cash. When denials rise, staff members burn themselves out, patient balances sit untouched, and growth stalls. This playbook provides a practical, step-by-step blueprint to move RCM from manual triage to autopilot so your team spends less time chasing dollars and more time running the practice.
In this playbook, you’ll learn how to:
Prevent avoidable errors before a claim ever goes out the door.
Submit claims faster and reconcile payments with real-time visibility.
Work denials in bulk with AI-generated appeals.
Collect patient responsibility with automated, patient-friendly payment workflows.
Key outcomes to highlight:
Faster cash flow (fewer days from visit to submission; fewer days in A/R).
Lower denial and rejection rates.
Higher patient responsibility collections with less staff effort.
Less rework and fewer “billing fire drills.”
Mid-market practices are stuck between enterprise complexity and lean-team reality.
Payer rules change. Staffing tightens. Patient responsibility rises. A small percentage of claims going sideways is a full-time job for your billing team. The result: unpredictable cash flow and a constant backlog of follow-up work.
Claim denials are rising
41%
of providers report denial rates of 10% or higher.
(Experian Health, 2025)
Denials often start with...
Data Issues
missing/inaccurate data and authorization issues remain major drivers. (Experian Health, 2025)
Patients are confused + stressed by coverage and bills
41%
have trouble understanding coverage.
58%
find paying a medical bill stressful.
(Ipsos, 2024; Cedar, 2024)
Clinicians spend substantial
Time on Paperwork
—time that should go to patients.
(Medscape/Becker’s, 2023)
Mid-market translation:
You can’t “hire your way out” of denials.
Every manual handoff is a new opportunity for errors.
The best RCM improvement is the one that happens inside existing workflows.
A claim should be a straight line. In reality, it’s a pinball machine.
Most RCM issues aren’t caused by one big mistake. They come from small gaps across the journey: registration errors, missed documentation, payer edits, and denial follow-up that never quite gets finished. "Work harder" often isn't enough. Clinicians need to make clean claims the default and rework the exception.
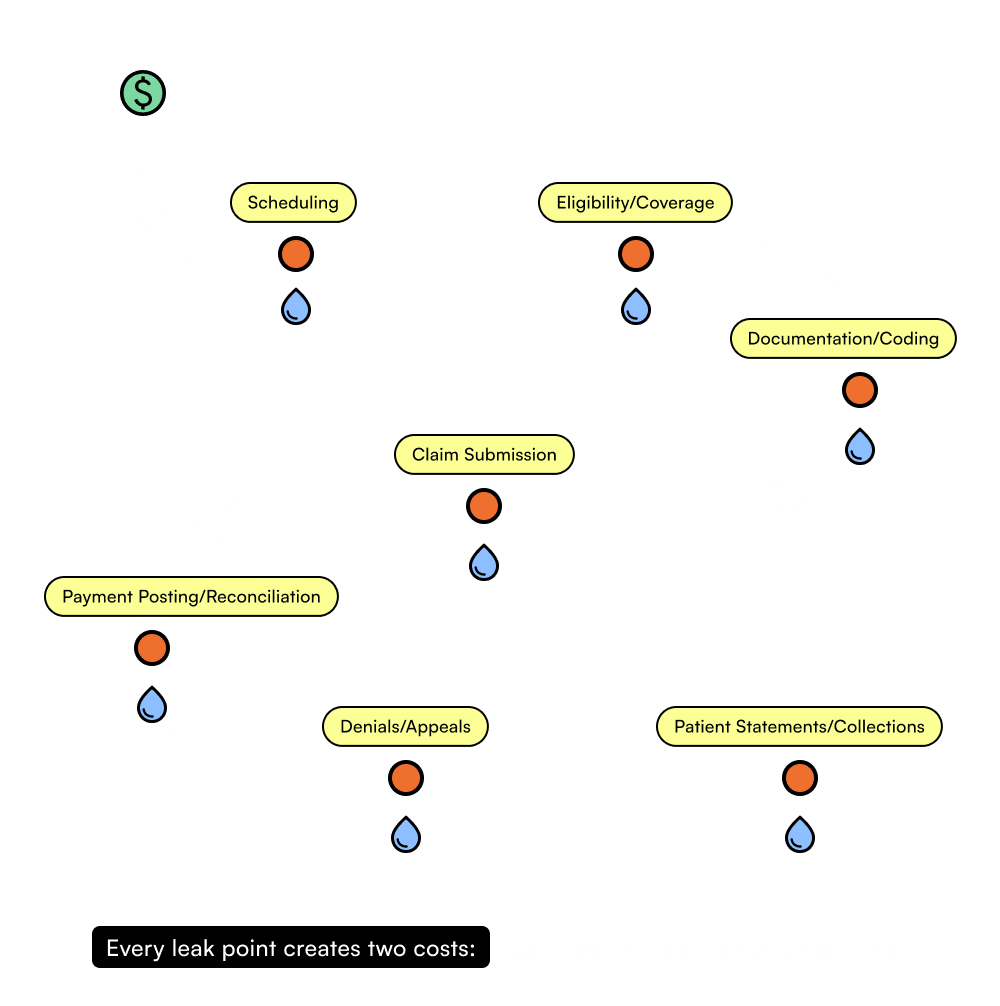
Four moves that make RCM feel… boring and predictable. (That’s a compliment.)
For mid-market organizations, the winning RCM strategy is repeatability. The goal is to reduce variability: fewer errors, fewer exceptions, fewer surprises. Here’s the blueprint we see in high-performing practices.
Start with clean data
Confirm workflows, billing needs, and your 90-day go-live plan.
Submit faster + reconcile live
Set up roles, templates, and run parallel validation—including 837 duplication for performance.
Fix denials at scale
Staff training (front desk, clinicians, billing) and guided go-live support.
Automate patient responsibility
Patient-friendly reminders, saved cards, and payment plans, without the awkward calls.
Clean Data In (Before the Visit Becomes a Denial)
Upfront accuracy: the cheapest denial prevention you’ll ever buy.
A surprising number of denials start as front-end problems: eligibility, coverage, and registration details that don’t match payer rules. When the data is wrong, the rest of the revenue cycle becomes expensive rework. The goal is simple: surface issues early when they’re easiest to fix.
How Athelas RCM supports this:
Coverage Detection: identify active insurance coverage to reduce avoidable coverage-related denials.
Standardized workflows that reduce manual variation across locations and staff.
Patient responsibility workflows that set clear expectations and reduce aging balances.
Eligibility verified (and documented)
Patient demographics match payer records
Correct payer + plan selected
(no duplicate/old coverage)
Patient balance workflow triggered
(estimate, reminders, payment method captured)
Submit Fast + Reconcile Live
Same-day submission isn’t a flex. It’s a cash-flow strategy.
The longer claims sit, the more they decay - missing codes, lost context, and higher risk of timely-filing issues. High-performing teams shorten the distance between care delivery and claim submission, then they monitor performance in real time.
Same-day claim submission
and live reconciliation with a claims engine that analyzes and optimizes each claim payload
Seamless EHR data pulls for billers
reduce double entry and screen switching so staff can work inside existing workflows
Real-time
transparency
dashboard views from high-level financials down to the individual claim level
AI-driven payment posting
to reduce manual posting errors and speed up processing
Denials & Appeals on Autopilot
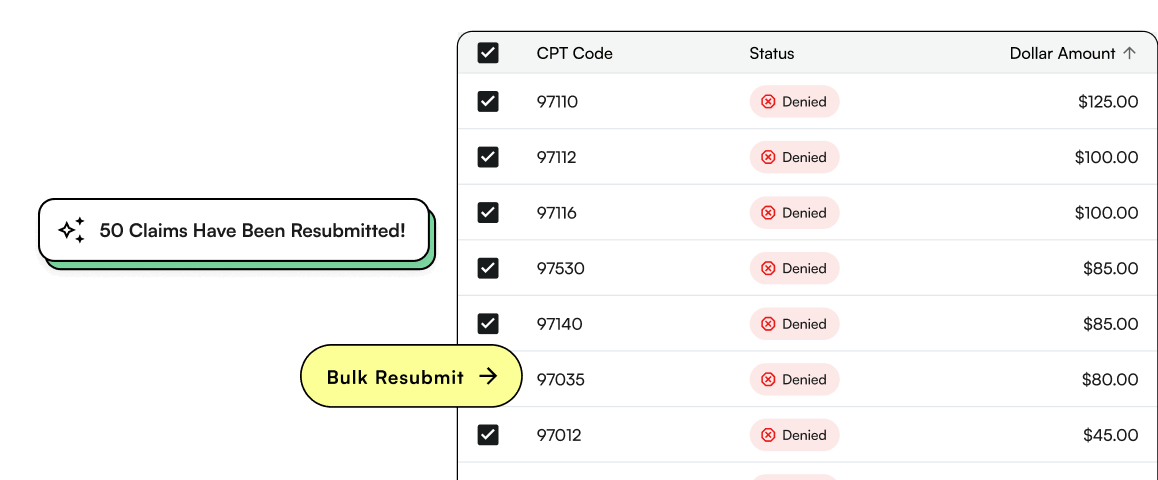
Denials shouldn’t be artisanal.
In a growing practice, denials pile up because they’re worked one at a time - with tribal knowledge trapped in a few people’s heads. The fix is to industrialize follow-up; bulk workflows, repeatable solutions, and AI help where it saves time.
Eligibility verified (and documented)
Authorization requirements confirmed when applicable
Patient balance workflow triggered (estimate, reminders, payment method captured)
Patient Responsibility
(Collected, Not Chased)
Make it easy to pay. Make it hard to forget.
Patient responsibility is a growing share of revenue, and it’s also the most awkward money to collect manually. The most consistent approach is consistent, automated, and respectful: clear reminders, easy payment options, and smart follow-up.
Multi-Channel Outreach
Automated reminders via text, email, and physical mail on pre-set cadences
Automated Collections
Auto-debit saved cards and failure reporting to increase collection rates with less effort
Flexible Financing
Payment plans (including Affirm) so you can get paid now while patients pay over time
A financial operating system that lives inside your daily workflow.
Athelas RCM is designed to integrate with your clinical system, reduce rework, and give your team real-time visibility. It’s not just a dashboard; it’s an operating layer that helps claims go out cleaner, get worked faster, and get paid more predictably.
Claims Engine
Optimizes claim payloads and supports same-day submission + live reconciliation.
RCM Insights Dashboard
Claim-level and practice-level visibility with one click.
Denial Copilot
Bulk resubmissions + standardized denial fixes.
AI Appeals
Draft, edit, and grade appeals at scale.
Patient Payments
Automated reminders, saved cards, and payment plans.
Integrations
Works with major EHRs.
From denials and write-offs to expansion.
Rockland Urgent Care faced credentialing and out-of-network denials, aging patient balances, and limited visibility into what was driving revenue leakage. With Athelas, they streamlined workflows, improved denial management, and strengthened patient collections.
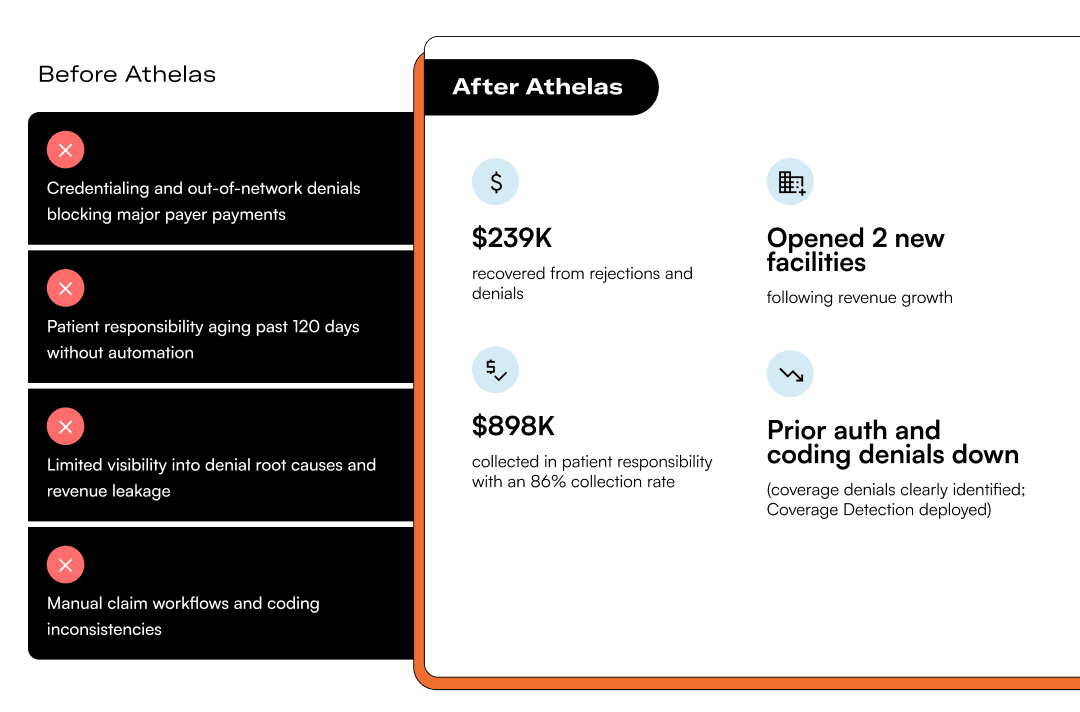
We simply don’t write off timely filing denials anymore.
— Kimberly Payton, Administrative Director
More visibility. Fewer denials. $3.6M/year growth.
Hillside Foot & Ankle needed better financial visibility and a path to scale beyond standard procedures. Athelas tailored rules across multiple business entities and delivered reporting that made performance clear and actionable.

It’s clear they genuinely care about supporting our practice.
— Dana Paris, Office Manager
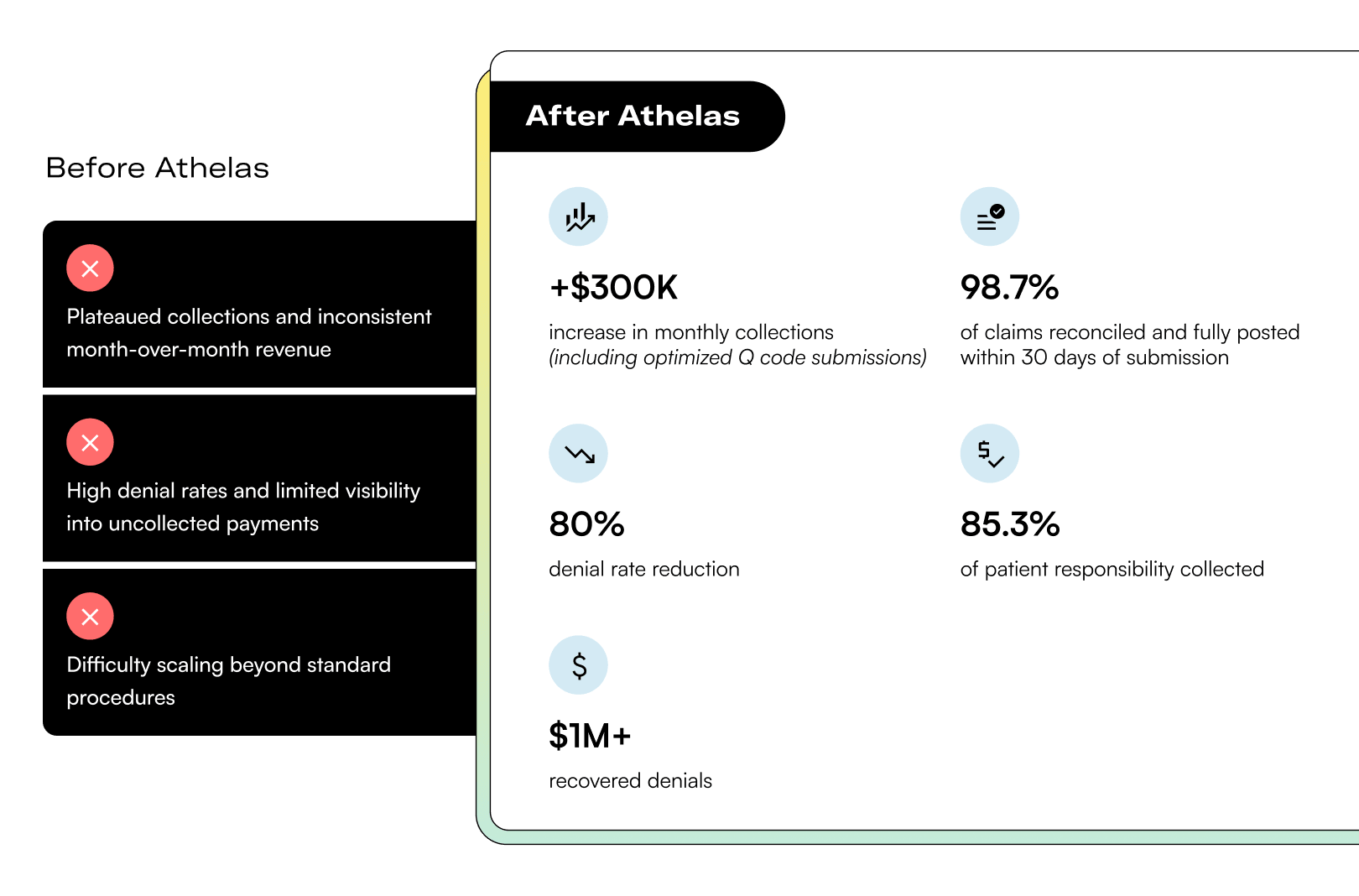
A denial and rejection rate of 2.2%—with faster submissions.
Springville, a multi-location specialty practice, wanted to reduce manual workflows, speed up reimbursements, and improve patient collections. With a rules-based automation approach and SmartPay workflows, they tightened performance across the cycle.
2.2%
denial/rejection rate (with 1.0% attributed to Athelas)
10 days
average time from date of service to submission (matching Athelas benchmarks)
90%
of patient responsibility collected; $50K+ collected in-office in recent months
34 Active Automations
ran by proprietary rules engine
$48k+
automatically recovered in recent denials
The human interaction component of Athelas is unmatched.
— Trent Wride, CEO
A rollout plan that won’t wreck your week.
Mid-market teams need speed and stability. Start with quick wins, then expand automation once workflows are steady. Below is a recommended 30/60/90 plan, plus the KPIs to review weekly.
Integrate with EHR
Validate data flows
Establish baseline metrics
Launch core dashboards
Turn on bulk denial workflows
Standardize top denial fixes
Implement patient payment cadences
Expand automations (payer rules, edits)
Optimize high-volume service lines
Tighten posting/reconciliation SLAs
Experian Health State of Claims Survey (2025); Ipsos (Oct 2024) on coverage understanding; Cedar 2024 Healthcare Financial Experience Study; Medscape/Becker’s (2023) paperwork hours; Athelas RCM product pages + published case studies.