Athelas Prior Authorization Automation for Orthopedics
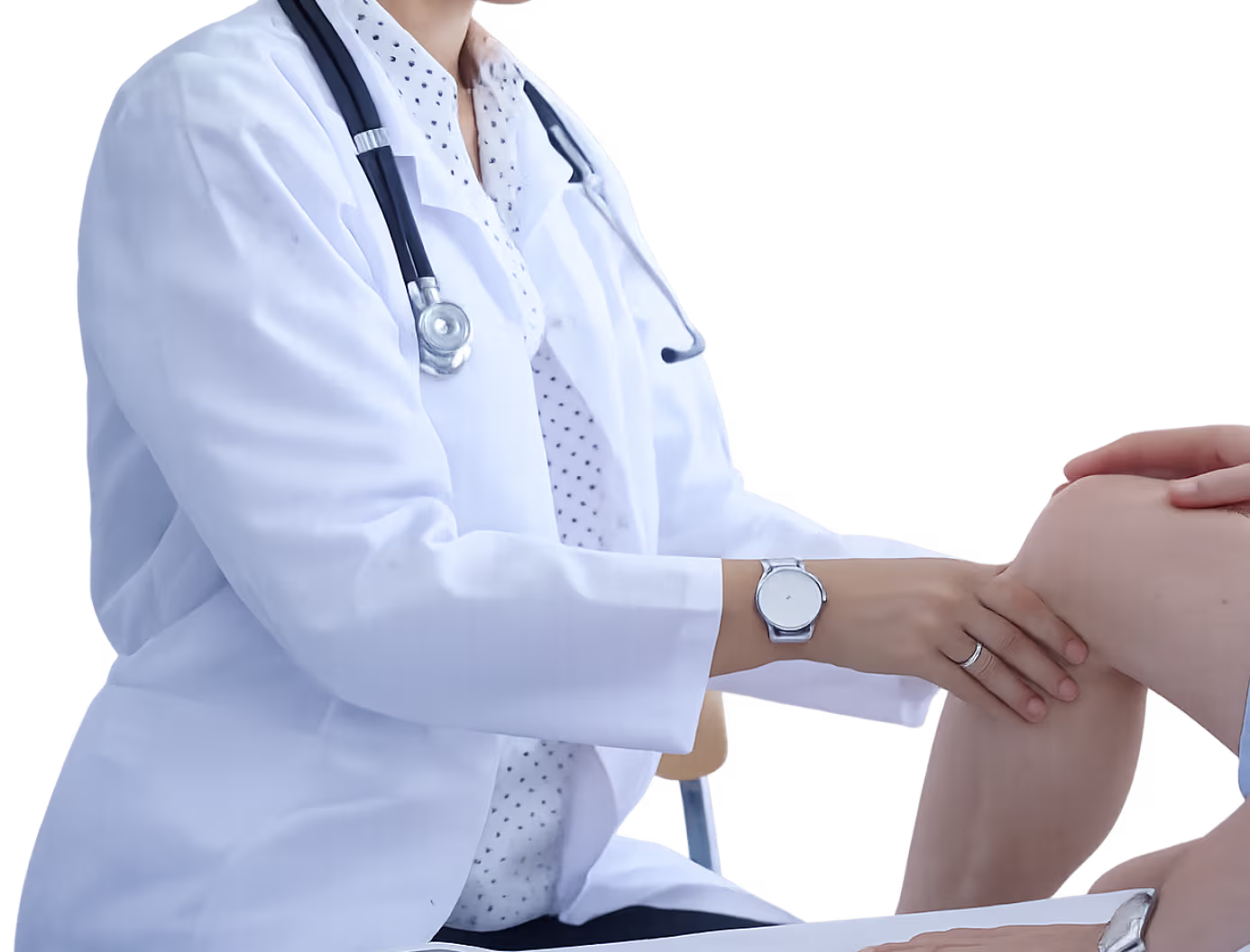
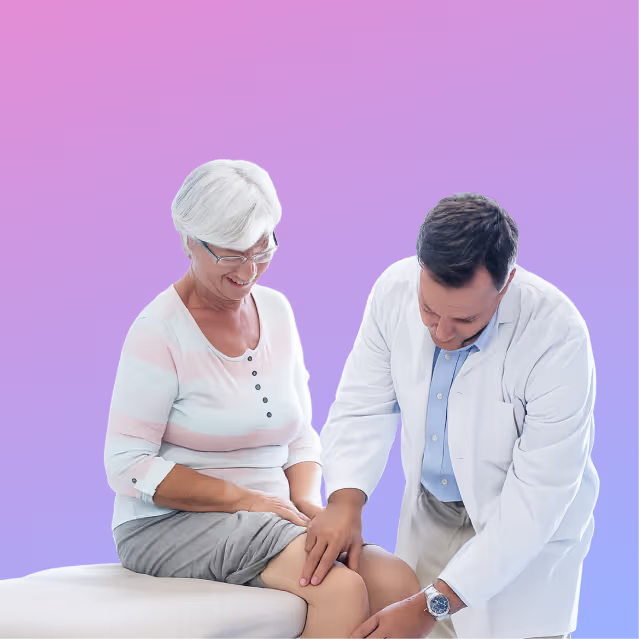

94% of physicians report care delays tied to prior authorization. Orthopedic surgeons rank among the specialties most impacted due to high imaging and procedural volume.
Practices complete an average of 45 prior authorizations per physician each week, and nearly 40% of staff time spent on authorizations is fully manual.
Prior authorizations (PAs) for imaging and procedures are a critical administrative step in orthopedic care that ensures payers approve necessary services before they are performed. When approvals are delayed or mishandled, imaging such as MRI and CT scans, joint injections, arthroscopy, and total joint procedures can be postponed, disrupting both patient outcomes and revenue timelines.
But when handled manually, prior authorizations take up significant staff time, require navigating multiple payer portals, and delay treatment and billing.
Athelas transforms prior authorization workflows so orthopedic practices can focus on care delivery instead of frustrating paperwork.
What Prior Authorization Means for Orthopedic Practices
A prior authorization confirms an insurer has signed off on a planned imaging study or orthopedic procedure before the service is rendered. In orthopedics, this often includes:
Imaging studies such as MRI, CT, or advanced diagnostic scans that require preapproval.
Elective or scheduled procedures that need clinical justification and insurer review.
Tracking authorization numbers, effective dates, and approved CPT codes.
High-volume orthopedic CPT codes that frequently require prior authorization often must include documentation of failed conservative treatment, imaging findings, and medical necessity criteria before approval is granted.
Without accurate and timely prior authorizations, claims can be denied, appointments may need rescheduling, and revenue can be delayed.
Common Challenges with Manual Prior Authorization
Orthopedic practices face specified pain points around prior authorization
Multiple payer systems require different forms or portal logins.
Imaging and procedure approvals involve detailed clinical documentation.
Follow-ups and status checks demand repeated calls or portal visits.
Missing or incorrect authorizations can become denials and appeal work.
The American Medical Association reports that physicians and staff spend an average of 12 hours per week completing prior authorizations, contributing significantly to administrative cost and burnout.
These challenges increase administrative burden, distract staff from patient engagement, and slow down revenue cycles.
How Athelas Prior Authorization Automation Helps
Athelas Agents include a dedicated Prior Authorization Agent that submits and tracks insurance approvals in real time. This AI-powered assistant works across payer portals to automate repetitive tasks and capture status updates, so staff spend less time on follow-up and data entry.
Faster, Smarter Submissions
The Prior Authorization Agent handles submission of requests for imaging and procedures, ensuring required patient, provider, and service information is entered accurately and routed through the correct payer channels.
Real-Time Tracking and Updates
AI automation takes over time-consuming tasks like tracking expiration dates, updating auth numbers, and checking payer responses. Practices can reallocate staff time to patient care and other high-value activities.
Reduced Administrative
Burden
AI automation takes over time-consuming tasks like tracking expiration dates, updating auth numbers, and checking payer responses. Practices can reallocate staff time to patient care and other high-value activities.
Improved Financial Outcomes
With prior authorizations submitted and tracked efficiently, orthopedic practices can reduce denials tied to missing or late approvals, protect revenue, and avoid rescheduling costs.
Better Patient Experience, Less Staff Friction
When authorizations are handled proactively, care stays on schedule. Patients experience fewer delays and clearer communication about what services are covered and approved. Staff can then focus on supporting patients and clinicians rather than chasing down insurer responses.
Athelas Prior Authorization Automation reduces administrative friction, improves payer communication, and supports practices in delivering high-quality care without sacrificing efficiency.
Built to Drive Revenue and Clarity for Your Practice


As orthopedics practices grow, revenue cycle complexity and lack of visibility into claims can slow everything down. Athelas is designed to support practices of all sizes with intelligent workflows that bring clarity and performance to financial operations.
Farnsworth Orthopedic Physical Therapy partnered with Athelas to get a real picture of their revenue cycle, boost collections, and eliminate surprises. With better insight and automation, they increased revenue by $14,000 every month, earned an extra $5 per encounter, and saw patient collections grow by $168,000 per year.
91% of their claims now require no manual intervention, less than 1% of denials go unworked, and only 7% of patient responsibility remains outstanding over time. Their success shows what’s possible when billing clarity and proactive management replace guesswork.
How Farnsworth Orthopedic Physical Therapy Increased Revenue by $14K Every Month
+$5 revenue
per encounter
$14K monthly
revenue growth
$168K/yr Increase
in patient collections
One Platform. Three Products. Working in Sync.
Athelas powers your practice with a unified platform
RCM Insights to accelerate payments and reduce denials.
Ambient AI to streamline documentation and support compliant coding.
Air EHR to connect front office, clinicians, and billing teams in real time.

We support you, so you can support patients.
That’s our promise.
Learn more about how Athelas can help your practice with Prior Authorizations.