Athelas Claims Scrubbing for Podiatry

Up to 15% of medical claims are initially denied, and industry estimates suggest that 50 to 65% of those denials are preventable.
The average cost to rework a denied claim exceeds $25, not including delayed cash flow or write offs. For podiatry practices managing high volumes of routine and medically necessary foot care, even small coding gaps can translate into significant revenue loss.


Certain podiatry codes face especially high scrutiny. CPT 11721 for debridement of six or more nails, CPT 11055 to 11057 for callus and corn paring, and routine foot care linked to ICD-10 codes frequently require precise documentation, modifier usage, and medical necessity support. Missing risk factors, incorrect modifiers, or frequency violations can quickly result in denials or downcoding.
What Claims Scrubbing Means for Podiatry Practices
Claims scrubbing reviews claims for accuracy and compliance before they are submitted to insurance. For podiatry, this often includes
Verifying diagnosis and procedure code alignment.
Confirming required modifiers and supporting documentation.
Checking payer specific rules for routine versus medically necessary care.
Identifying services that require additional justification.
Ensuring claims meet frequency and coverage requirements.
Because podiatry services are frequently scrutinized by payers, even minor inconsistencies can result in denials or downcoding.
Routine vs Medical Necessity Complexity
Podiatry claims often hinge on whether a service is considered routine or medically necessary. This distinction is one of the most common sources of denials.
Routine foot
care rules
Many payers do not cover routine foot care unless strict criteria are met. Nail trimming, callus care, and similar services often require specific diagnoses and documentation to be considered covered.
Medical necessity documentation
Conditions such as diabetes, peripheral vascular disease, or neuropathy can support medical necessity, but only when documentation clearly supports the diagnosis and risk factors. Missing details or mismatched codes can trigger denials.
Frequency
limitations
Even when care is medically necessary, payers may limit how often certain services can be billed. Claims outside allowed frequency windows are often denied automatically.
Common Challenges with Manual Claims Scrubbing
Podiatry practices face recurring challenges when reviewing claims by hand
denials after submission.
supporting documentation.
routine care rules across payers.
medical necessity criteria.
rejections.
Given that denied claims can take weeks to resubmit and often result in partial reimbursement, preventable errors directly impact operating margin and staff productivity. These issues impede cash flow and create unnecessary work for your billing team.
How Athelas Supports Claims Scrubbing for Podiatry
Athelas supports podiatry practices with a modern platform designed to catch issues before claims are submitted.
Proactive claim risk detection
RCM Insights highlights patterns tied to denials, including routine care exclusions and medical necessity gaps. Practices can address issues earlier instead of reacting after payment delays.
Documentation and coding alignment
With Athelas Air and Ambient workflows, documentation and coding stay connected. This helps ensure diagnoses, procedures, and modifiers support one another before claims are finalized.
Consistency across payers
Athelas helps standardize claims review across payer rules, reducing variability and missed requirements that commonly lead to denials.
Fewer Denials,
Faster Payments
Cleaner claims mean fewer rejections, less rework, and faster reimbursement. By catching routine versus medical necessity issues upfront, podiatry practices can submit claims with confidence and reduce time spent on appeals and follow ups.


Fewer Denials,
Faster Payments
Athelas helps practices scale by bringing precision and visibility to the revenue cycle, no matter how complex the organization becomes. Hillside Foot & Ankle used Athelas to dramatically improve collections and regain control of denied revenue. They reduced denials by 80%, recovered over $1 million in lost revenue, and increased monthly collections by $300,000. With nearly all claims posted within 30 days and stronger patient responsibility collection rates, Hillside gained the financial clarity needed to grow with assurance.
How Hillside Foot & Ankle Grew Their Business by $3.6M/Year with Athelas
+$300k
increase in monthly collections
80%
increase in monthly collections
$1m+
recovered denials
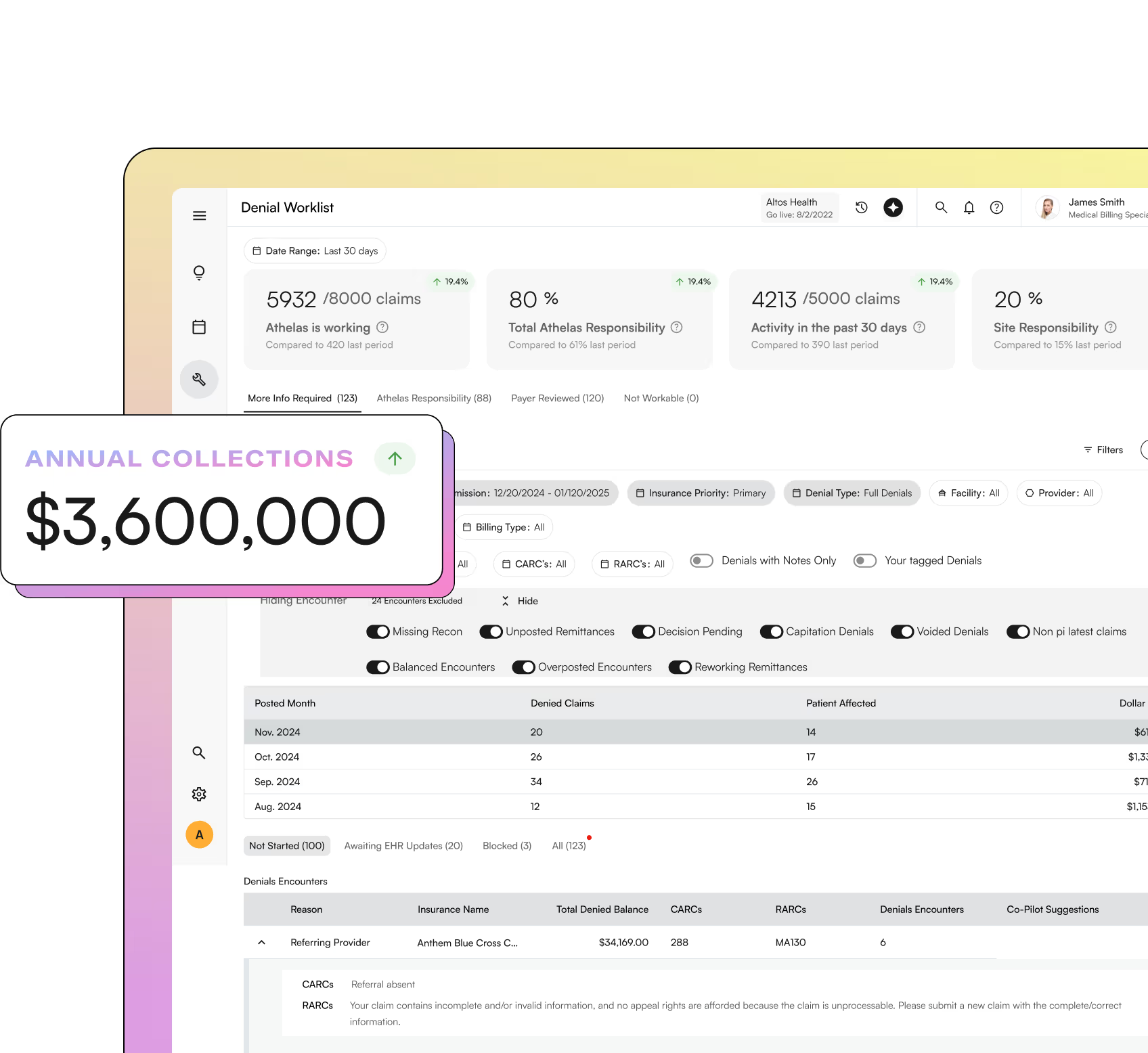
Athelas brings claims, documentation, and revenue operations into one interconnected system
RCM Insights to reduce denials and speed up payments.
Ambient tools to support accurate, compliant documentation.
Air EHR to connect clinical and billing teams in real time.
Claims scrubbing should protect your revenue and help your teams move faster. When denial prevention is built into documentation and coding workflows, practices spend less time correcting errors and more time delivering care.
Less time fixing revenue issues.
More time treating patients.
Learn more about how Athelas can support claims scrubbing for your podiatry practice.